Breast Reduction and Tummy Tuck — Complete Body Contouring After Weight Loss
Dr. Harikiran Chekuri, a Plastic Surgeon in Hyderabad, performed a combined breast reduction and abdominoplasty on a patient with post-weight loss body changes including breast ptosis and abdominal skin laxity. The procedure, done under general anesthesia, addressed sagging breasts, diastasis recti, and excess abdominal skin in a single session. The patient reported high satisfaction with excellent body contouring results. Post-operative swelling and temporary discomfort were the only expected side effects, with no complications reported.
PATIENT PROFILE
PARAMETER | DETAIL |
Age | 36 years |
Gender | Female |
Occupation | Doctor (Neurologist) |
City | Hyderabad, India |
Presenting Complaint | Saggy breasts with downward pointing nipples, loose abdominal skin with persistent lower belly bulge despite exercise |
Diagnosis | Breast Ptosis with Macromastia, Abdominal Skin Laxity with Diastasis Recti |
Duration of Issue | Progressive changes following pregnancies and weight fluctuations |
Previous Treatments | Diet and exercise — no surgical intervention prior |
Date of Procedure | February 2026 |
Outcome | Excellent — balanced body contour achieved |
THE PROBLEM
Sandhya came to us with two related concerns that had been bothering her for years. Her breasts had become heavy and saggy after pregnancies and weight changes. The nipples were pointing downward. Finding bras that fit properly was a daily struggle, and the weight of her breasts caused neck and shoulder discomfort.
Her abdomen told a similar story. Despite regular exercise and a controlled diet, she had loose hanging skin around her lower belly. Stretch marks covered much of the area. There was also visible muscle separation diastasis recti that made her stomach bulge outward even when she was at a healthy weight. Her core felt weak, and nothing she tried at the gym seemed to fix it.
As a neurologist who meets patients daily, Sandhya wanted to feel comfortable in her own body again. She had done the work the diet, the exercise, the discipline. But some things just do not respond to lifestyle changes alone. The loose skin was not going anywhere. The muscle separation could not be fixed with crunches. She needed a surgical solution.
CONSULTATION & TREATMENT PLAN
WHAT WAS ASSESSED DURING THE CONSULTATION
Dr. Harikiran Chekuri conducted a thorough pre-operative evaluation covering all clinical and personal parameters:
- Degree of breast ptosis — confirmed Grade 3 with nipples well below the inframammary fold
- Breast volume and skin quality — excess glandular tissue with stretched skin envelope
- Abdominal skin laxity — significant excess skin below the umbilicus with stretch marks
- Rectus diastasis — palpable muscle separation along the midline
- Patient goals — proportionate breasts, flat abdomen, improved body contour
- Medical fitness — cleared for general anesthesia and combined surgery
WHY COMBINED SURGERY WAS CHOSEN
- Single anesthesia session reduces overall surgical risk compared to two separate procedures
- One recovery period instead of two less total downtime for a working professional
- Better aesthetic planning breasts and abdomen can be balanced together for proportional results
- Breast reduction addresses ptosis, reduces volume, and repositions nipples to a natural height
- Abdominoplasty removes excess skin, tightens the abdominal wall, and repairs diastasis recti
PRE-OPERATIVE PHOTOS
Before the procedure, Dr. Harikiran Chekuri made precise pre-operative markings with the patient standing upright. These markings define the midline, inframammary fold, breast footprint, areas for liposuction, and the abdominoplasty incision line a critical step for bilateral symmetry and accurate tissue removal.
PRE-OP — FRONTAL VIEW WITH SURGICAL MARKINGS
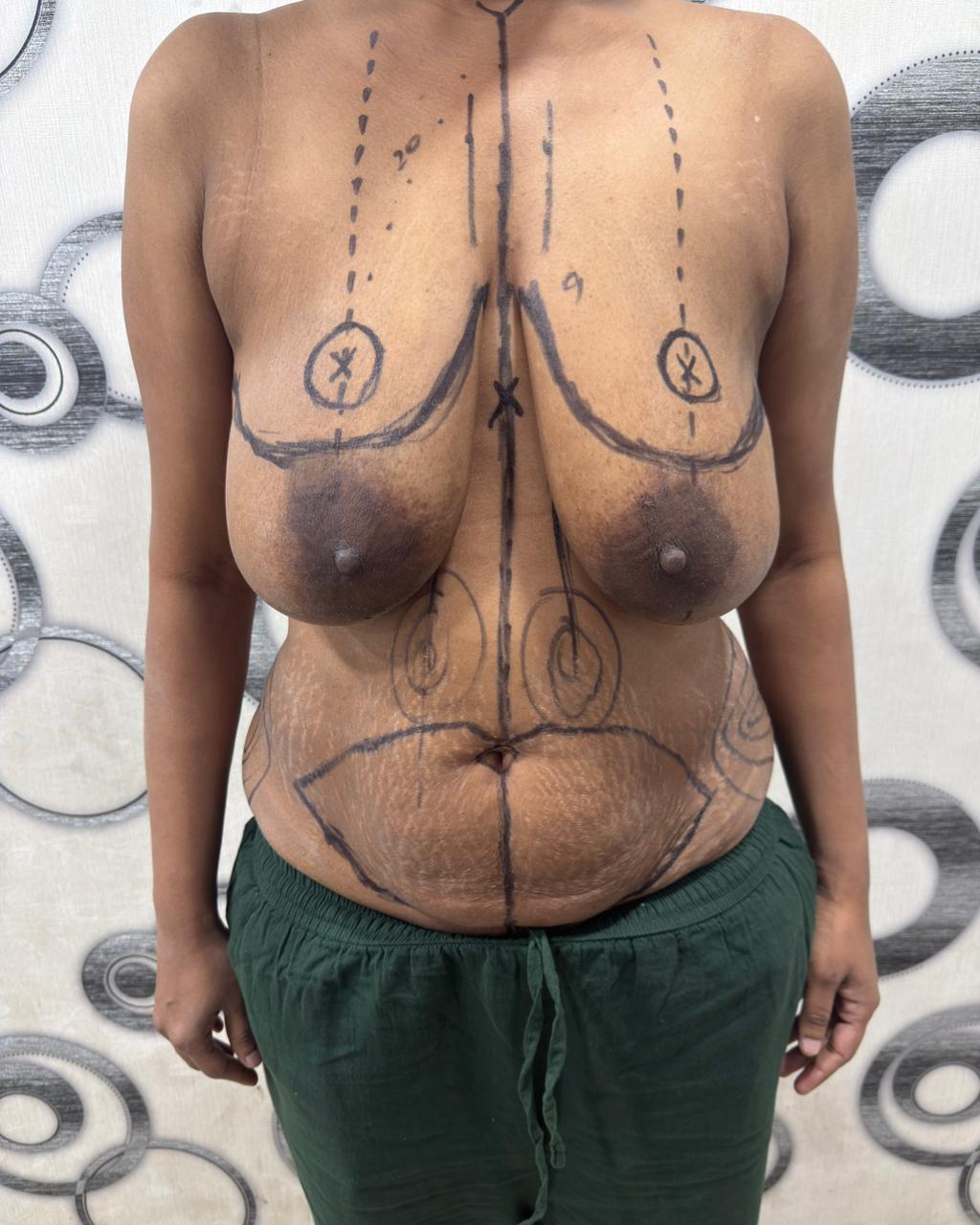
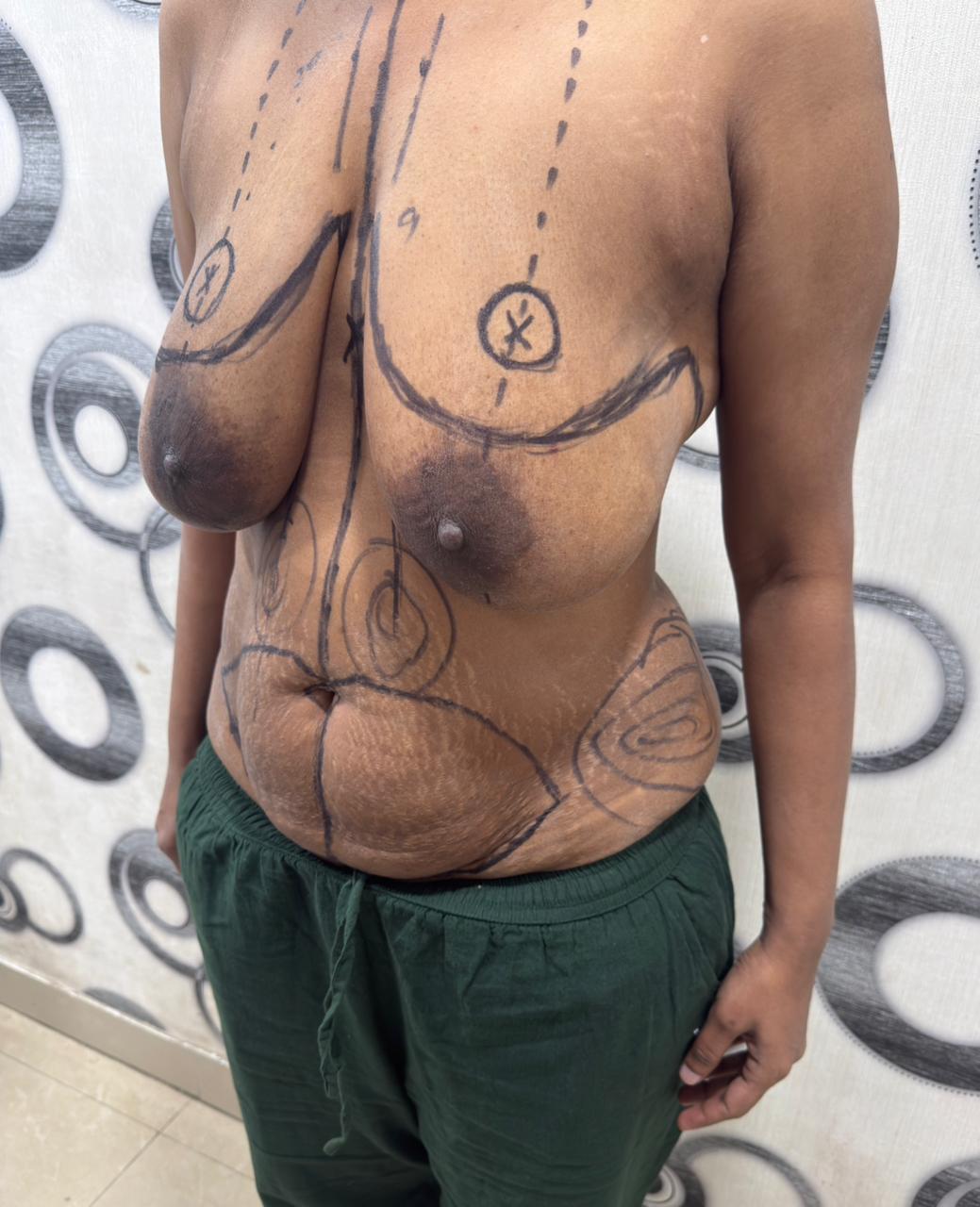
PRE-OP — LATERAL VIEW
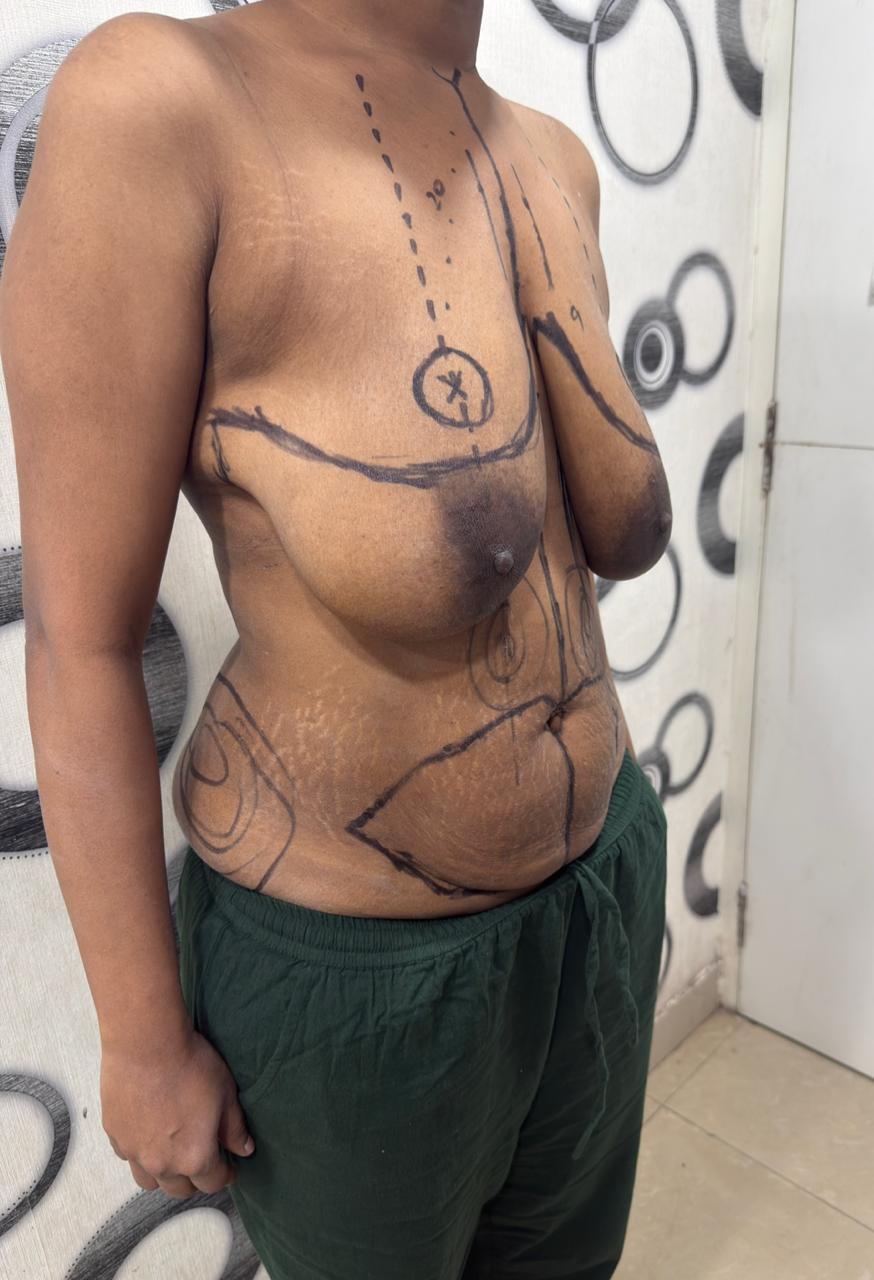
PROCEDURE DETAILS
- Pre-operative markings finalized with patient standing — breast footprint, nipple position, and abdominal incision line confirmed
- General anesthesia administered — patient fully asleep and monitored throughout
- Breast reduction performed first — excess glandular tissue and skin removed bilaterally
- Nipple-areola complex repositioned to a natural height while maintaining blood supply
- Breast incisions closed in layers with fine sutures — anchor pattern incision used
- Abdominoplasty incision made along the lower abdomen — excess skin undermined and excised
- Rectus muscles plicated along the midline to repair diastasis recti and flatten the abdominal wall
- New umbilicus created at the appropriate position
- Drains placed bilaterally for fluid management — abdominal incision closed in layers
- Compression garment and surgical bra applied before transfer to recovery
PROCEDURE FACTS
PARAMETER | DETAIL |
Duration | Approximately 4–5 hours (combined procedure) |
Anesthesia | General anesthesia — patient asleep throughout |
Procedures Performed | Breast Reduction (bilateral) + Abdominoplasty with Diastasis Repair |
Incision Type | Anchor incision (breast) + Low transverse incision (abdomen) |
Intraoperative Complications | None |
Hospital Stay | 1–2 nights observation |
POST-OPERATIVE RESULTS — IMMEDIATE
The images below show the immediate post-operative result in the operating room. The breasts are lifted to a natural position with reduced volume. The abdomen is flat with a low transverse scar and a newly positioned umbilicus. Drains are in place for fluid management. Swelling is expected and will settle over the coming weeks.
IMMEDIATE POST-OP — FRONTAL & LATERAL VIEWS
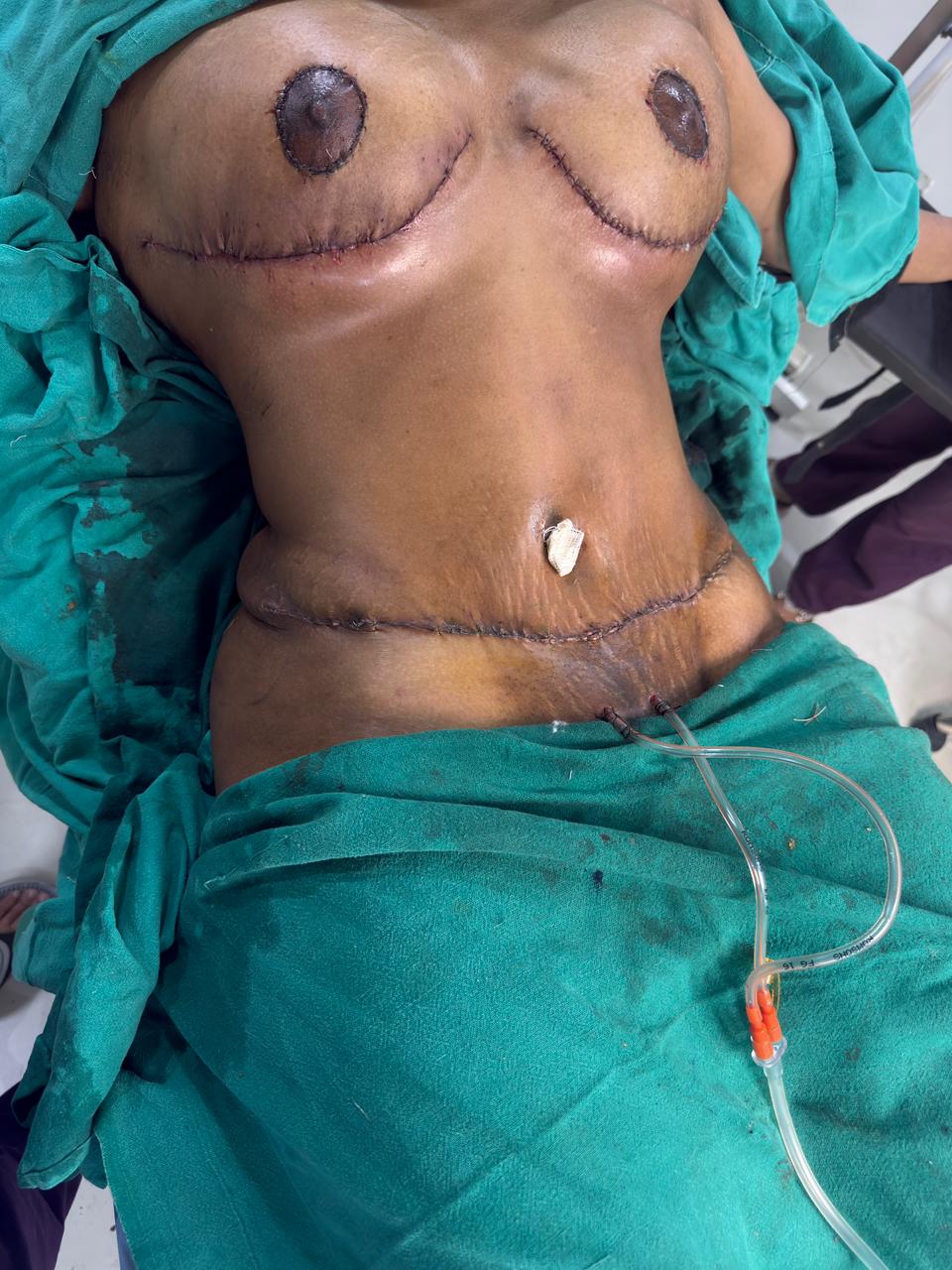
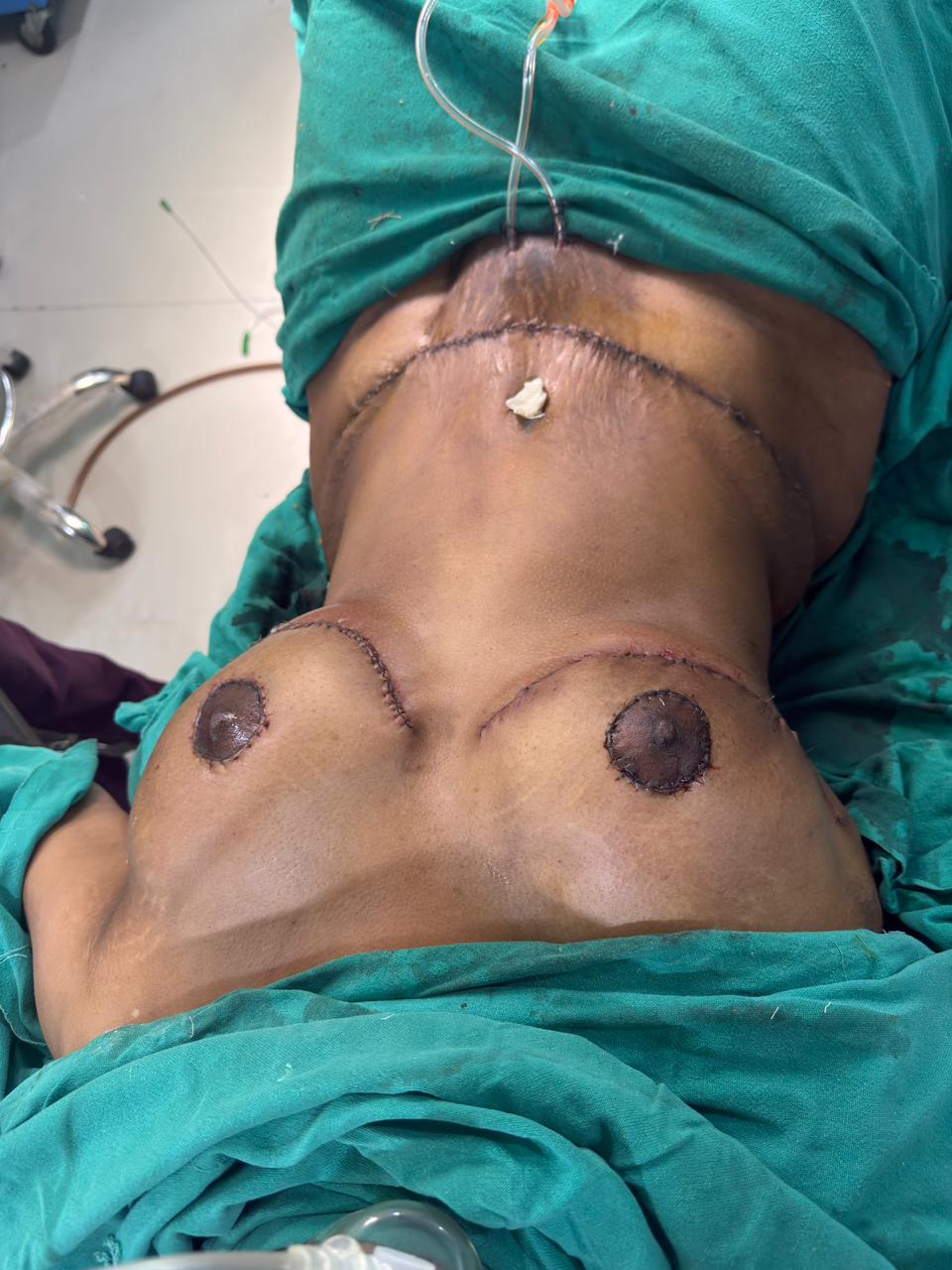
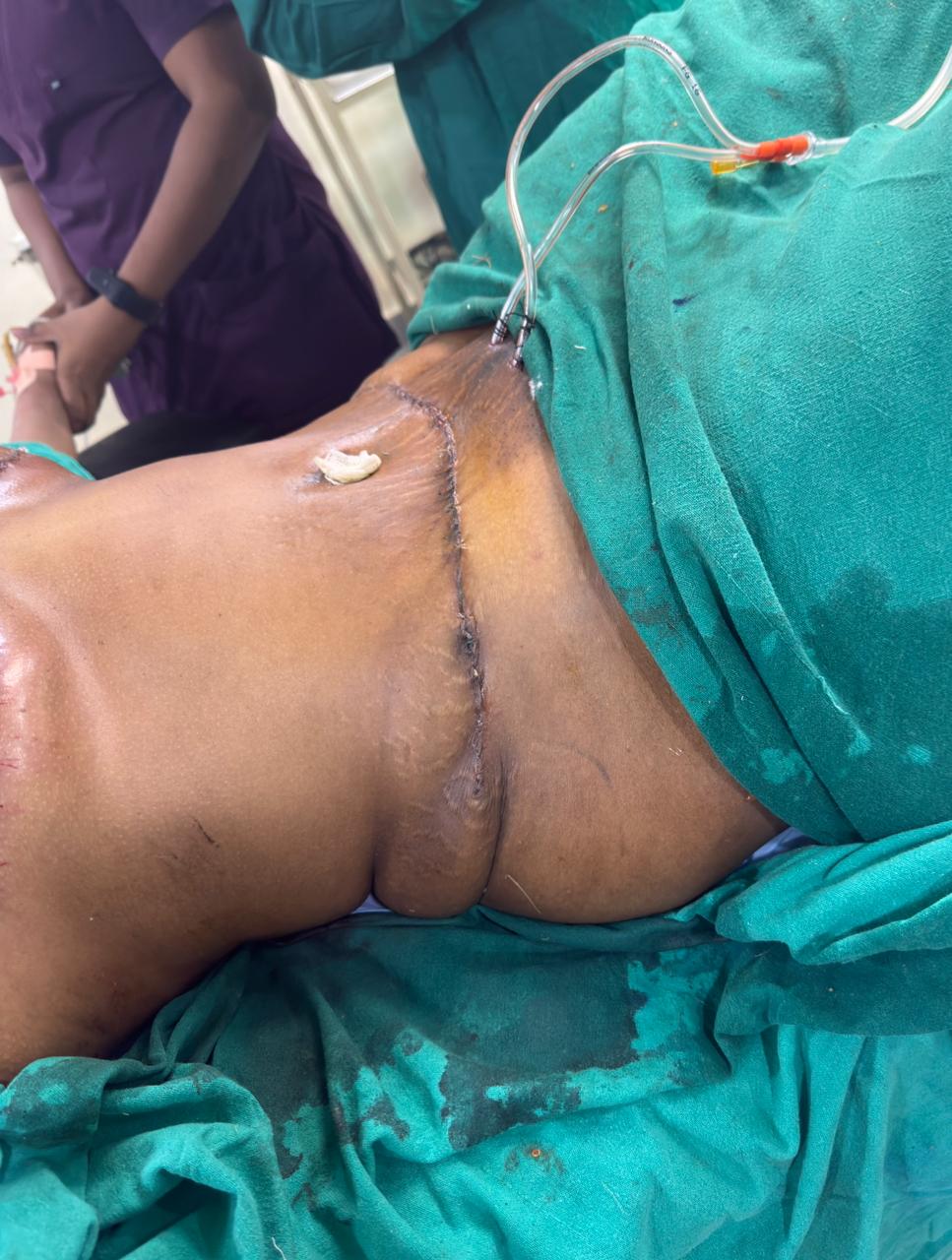
OUTCOMES AT A GLANCE
OUTCOME METRIC | RESULT |
Breast Symmetry | Excellent — bilateral balance achieved |
Abdominal Contour | Flat — excess skin removed, muscles repaired |
Patient Satisfaction | Very high — renewed confidence reported |
Complications | None |
Recovery | Smooth — within expected timeline |
PATIENT FEEDBACK
Feedback was recorded during the patient’s post-operative follow-up at Redefine, Gachibowli. The patient had been closely monitored through her recovery and offered the following observations.
POST-PROCEDURE CARE & RECOVERY
- Wear the prescribed compression garment and surgical bra continuously as advised to reduce swelling and support healing
- Avoid heavy lifting, strenuous activity, and core exercises for at least 4–6 weeks
- Keep the incision areas clean and dry — follow wound care instructions strictly
- Watch for redness, discharge, or fever — report any concerns immediately
- Sleep on your back with your upper body slightly elevated to reduce swelling and tension on sutures
- Walk gently from day one to improve circulation — avoid sudden movements or stretching
- Attend all follow-up visits and take medications exactly as prescribed
RECOVERY TIMELINE
TIMEFRAME | WHAT TO EXPECT |
Days 1–3 | Soreness and swelling. Rest recommended. Walk short distances. Drains managed. |
Week 1–2 | Swelling reduces. Drains removed. Suture check. Light desk work possible. |
Week 4–6 | Daily activities resume. Compression garment may be reduced. Light walking. |
Month 3 | Final result largely visible. Light exercise reintroduced. Scars fading. |
Month 6–12 | Full outcome confirmed. Scars mature. Long-term results established |

